Introduction
In today’s fast-paced world, heart failure has become common. According to the CDC, this affects around 64 million people worldwide. Heart failure occurs when the heart muscle weakens or stiffens, affecting its ability to pump blood efficiently. This results in fluid build-up, causing congestion in the body parts.
When heart failure occurs on the right side, it causes fluid buildup in the abdomen and lower extremities. In contrast, left-side failure leads to fluid accumulation in the lung, resulting in shortness of breath problems.
Congestive heart failure (CHF) is sometimes used synonymously with heart failure since the symptoms of both right- and left-sided heart failure include congestion.
Moreover, conditions like high blood pressure and narrow arteries impact heart working procedures, leading to a weakened heart and a high risk of heart failure.
Early medical treatment is very beneficial in managing symptoms and reducing complications. Lifestyle also makes a huge difference in your heart health; small changes like regular exercise, proper meals, weight loss, reduced salt intake, and stress management can improve your quality of life.
Types Of Heart Failure

| Types | Description | Key Symptoms | Causes |
| Left-side heart failure | The left ventricle is not able to pump blood properly, causing fluid buildup in the lungs | Shortness of breath, coughing, fatigue, fluid in the lungs | High blood pressure, coronary artery disease, heart attack |
| Right-side heart failure | The right ventricle fails to pump blood to the lungs leading to blood retention. | Swelling in legs, ankle, abdomen, bloating, weight gain | Left-side heart failure, lung disease, heart valve disease |
| Diastolic heart failure | Stiff heart muscle and doesn’t fill with blood properly | Shortness of breath, swelling, high blood pressure | Aging, obesity, diabetes, hypertension |
| Systolic heart | Heart muscle | Fatigue, shortness of | Heart attack, |
| Failure | weakens and cannot contract properly, reducing blood ejection | breath, reduced exercise tolerance | hypertension, cardiomyopathy |
| Acute Heart Failure | Sudden onset, often due to a medical surgery | Severe shortness of breath, rapid weight gain, confusion | Heart attack, infection, fluid overload |
| Chronic Heart Failure | Long-term conditions that worsen over time but can be managed | Gradual worsening of symptoms, fatigue, swelling | High blood pressure, coronary artery disease, lifestyle factors. |
Symptoms Of Heart Failure
| Category | Symptoms | Description |
| Respiratory Symptoms | 1. Shortness of breath 2. Persistent coughing or wheezing | 1. Difficulty breathing, especially during activity or lying down. 2. Due to fluid buildup in the lungs |
| Circulatory Symptoms | 1. Fatigue and weakness 2. Rapid or irregular heartbeat | 1. Reduced blood flow leads to tiredness 2. The heart compensates for weak pumping |
| Fluid Retention Symptoms | 1. Swelling in legs, ankles, feet 2. Sudden weight gain 3. Abdominal bloating or pain | 1. Due to fluid build-up from poor circulation. 2. Fluid accumulation in the body. 3. Caused by fluid buildup in the abdomen. |
| Neurological Symptoms | 1. Confusion or difficulty in concentration 2. Dizziness or fainting | 1. Reduced oxygen-rich blood supply to the brain. 2. poor circulation or low BP |
| Other Symptoms | 1. Increase urination at night 2. Reduced exercise tolerance | 1. The body tries to remove excess fluid while resting. 2. Weakness or breathlessness during activity. |
Causes Of Heart Failure
- Coronary Artery Disease (CAD) – Narrowed or blocked arteries reduce blood supply to the heart.
- High Blood Pressure (Hypertension) – Forces the heart to work harder, weakening it over time.
- Heart Attack (Myocardial Infarction) – Causes permanent damage to the heart muscle, affecting its ability to pump.
- Cardiomyopathy – Disease of the heart muscle due to genetics, infections, alcohol, or drug abuse.
- Valvular Heart Disease – Damaged heart valves strain the heart by causing inefficient blood flow.
- Arrhythmias (Irregular Heartbeat) – Disrupts normal heart function, reducing pumping efficiency.
- Diabetes – Increases the risk of high blood pressure and coronary artery disease.
- Obesity – Puts extra strain on the heart, increasing heart failure risk.
- Thyroid Disorders – Overactive or underactive thyroid can weaken the heart.
- Chronic Kidney Disease – This leads to fluid retention and increased strain on the heart.
- Excessive Alcohol or Drug Use – Weakens heart muscle over time.
- Congenital Heart Defects – Structural heart abnormalities present from birth can cause failure later in life.
- Sleep Apnea – Interrupts oxygen supply, increasing heart strain.
- Severe Lung Diseases (COPD, Pulmonary Hypertension) – Make it harder for the heart to pump blood effectively.
- Infections (e.g., Viral Myocarditis) – Can inflame and damage the heart muscle
Difference Between Heart Failure And Congestive Heart Failure
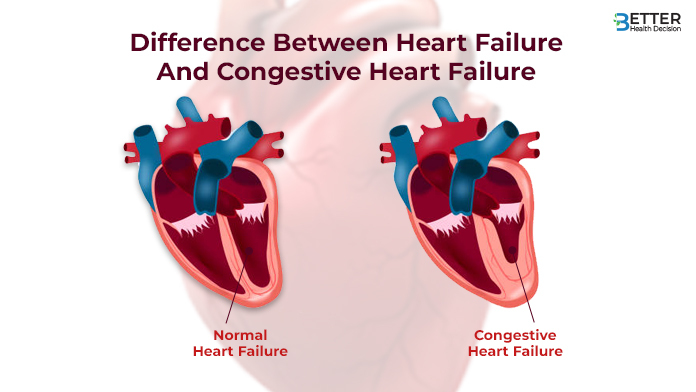
| Feature | Heart Failure | Congestive Heart Failure |
| Definition | Condition in which the heart struggles to pump blood effectively | The advanced stage of heart failure is when fluid gets stored in different body parts |
| Cause | It can be caused by high blood pressure, previous heart attack, or coronary artery disease. | Occurs when heart failure causes fluid accumulation in the lungs, legs, and other body organs. |
| Symptoms | Rapid heartbeat, breath shortness, restlessness, fatigue | Swelling in ankles, legs, fluid retention, severe shortness of breath, coughing. |
| Fluid Buildup | May or may not have fluid retention | Fluids always build up in the lungs or other organs. |
| Severity | It can be mild or severe | Advanced and severe forms of heart failure. |
| Treatment | Healthy lifestyle, regular checkups, proper medication | Require intensive treatment, including diuretics and possible hospitalization. |
When To See A Doctor?
If you have any symptoms, you should consult your doctor.
Emergency Symptoms (Seek Immediate Medical Help):
- Severe shortness of breath (especially at rest or lying down)
- Chest pain or pressure
- Fainting or severe dizziness
- Rapid or irregular heartbeat accompanied by weakness
- Sudden and severe swelling in the legs, feet, or abdomen
- Pink, frothy sputum when coughing (a sign of fluid in the lungs)
Some other symptoms that should not be ignored:
- Breathlessness during daily activities.
- Continuous fatigue and weakness.
- Frequent swelling in the ankles, feet, or abdomen.
- If you have gained weight instantly.
- Frequent nighttime urination (nocturia)
- Persistent cough or wheezing
Such changes could mean that heart disease is getting worse and treatment is not working.
How Heart Failure Is Diagnosed?
A doctor starts by performing a physical exam and assessing your medical history to check for signs of heart failure.
1. Medical History & Physical Exam
- Review symptoms (shortness of breath, fatigue, swelling, etc).
- Checking for risk factors like high blood pressure, diabetes, or heart disease
- Listening to the heart and lungs for abnormal sounds.
2. Diagnostic Tests
- Blood Tests – Check for heart-related markers like BNP (B-type Natriuretic Peptide) levels.
- Electrocardiogram (ECG/EKG) – Detects irregular heart rhythms or past heart damage.
- Chest X-ray – Identifies fluid buildup in the lungs and heart size.
- Echocardiogram – Uses ultrasound to assess heart structure, function, and ejection fraction (EF).
- Stress Test – Evaluates how the heart responds to exertion.
- Cardiac MRI or CT Scan – Provides detailed images of the heart.
- Cardiac Catheterization (Angiography) – Checks for blocked arteries affecting heart function.
How Is Heart Failure Treated?
Treating heart failure depends on its severity and type. Early treatment can quickly improve symptoms, but regular checkups and monitoring every six months are essential. The primary goal of therapy is to enhance lifespan, prevent complications, and improve overall quality of life through medications, lifestyle changes, and medical interventions.
Heart failure treatment focuses on improving heart function, managing symptoms, and preventing complications. It includes lifestyle changes, medications, medical devices, and surgeries.
1. Lifestyle Changes
Small changes in your lifestyle can improve your heart health and reduce the risk of heart failure:
- Lessen salt intake
- Regular physical exercise
- Weight management
- Quit alcohol and smoking
- Getting proper sleep and rest
2. Medications
Medications may treat early stages of heart failure. They can help relieve your symptoms and prevent your condition from worsening.
Some medicines are prescribed to :
- remove excess fluid to reduce swelling
- improve your heart’s ability to pump blood
- reduce blood clots
- reduce your heart rate when necessary
- remove excess sodium and replenish potassium levels
- reduce cholesterol levels
- reduce adverse hormones and reactions in your body that can weaken your heart.
These medications can include:
- Beta-blockers
- ACE inhibitors
- Water pills
- Digoxin
- Blood thinners
- Cholesterol-lowering
- Aldosterone Antagonists
- SGLT2 inhibitors
Consult your doctor before starting any new medication. People with heart failure are recommended to avoid some medicines that are allergic, such as nonsteroidal anti-inflammatory drugs(NSAIDs); these can further worsen fluid retention in heart failure.
3. Medical Devices
-Pacemaker
A pacemaker is a small device implanted in the chest to control abnormal heartbeat. Sending electrical signals ensures the heart beats at regular rates. The pacemaker helps in sensing the heartbeat and helps prevent dizziness, fatigue, and fainting caused by slow or irregular heartbeats, improving overall heart function.
-Implantable Cardioverter Defibrillator (ICD)
It is a powered device placed under the skin to monitor and regulate abnormal heartbeat( arrhythmias). Through its electrical waves, it continuously monitors heart activity. It delivers shock or pulse if it detects irregular rhythms like ventricular tachycardia or ventricular fibrillation, which can cause sudden cardiac attack. ICDs improve survival in individuals who are at high risk of heart failure by reducing the risk of sudden cardiac arrest.
-Cardiac Resynchronization Therapy (CRT)
CRT is a specialized treatment that helps in the coordination of heart ventricles. In some heart patients, the left and right ventricles do not work in sync, and because of this, the heart cannot pump correctly, resulting in reduced heart efficiency. A CRT sends electrical signals to both ventricles to help them contract simultaneously, improving blood flow and oxygen delivery throughout the body. This therapy helps reduce shortness of breath, fatigue, and swelling by improving heart functionality.CRT is often used in patients with moderate to severe heart failure and an abnormal heart rhythm, known as left bundle branch block (LBBB).
-Left Ventricular Assist Device (LVAD)
A left ventricular assist device (LVAD) is a mechanical pump that helps pump blood effectively. This device is planted in patients with severe heart failure who are not eligible for transplantation. It is implanted inside the patient’s chest, with one end attached to the heart’s main pumping chamber (the left ventricle) and the other connected to the aorta (the main artery that carries blood). The battery pack and the control unit remain outside the body to power the device.
How Can You Prevent Heart Failure?
- Have a healthy and balanced diet
- Regular physical exercise
- Maintaining a moderate weight
- Limit alcohol intake
- Avoid smoking
- Get proper sleep
- Get regular medical checkups
- Limit sugar intake
Complications Of Heart Failure
If heart failure is not treated timely, it can result in chronic heart failure(CHF), in which blood starts storing in the other parts of the body, and it can be life-threatening. You may experience fluid retention in your limbs and organs like the liver and lungs.
- Stroke
- Kidney dysfunction
- Liver dysfunction
- Thromboembolism (blood clots)
- Arrhythmias, such as ventricular arrhythmias
- Heart attack
Early diagnosis and proper management can help reduce the risk of these complications.
Overview
When the heart cannot pump enough blood to meet the body’s needs, the body starts experiencing fatigue, shortness of breath, and fluid retention leading to heart failure. It is a chronic disease that needs medical treatment to prevent it from worsening and to improve quality of life. The severity and treatment depend on the type of heart failure; early diagnosis stops further progression. A healthy lifestyle and seeking early treatment can enhance heart health significantly, promoting your overall health.
Frequently Asked Question
1- What are the possible signs that the heart is failing quietly?
Heart failure does not develop instantly and may not show visible symptoms initially. But it starts occurring slowly, and sometimes it is hard to recognize. But sure signs start giving indications like:
- Fatigue
- Dizziness
- cough
- Edema
- Shortness of breath
- Reduced stamina
If you start noticing these signs in your body, then consult your doctor for a checkup.
2 – Can we detect congestive heart failure through blood tests?
Yes, congestive heart failure can be detected through blood tests, initially by measuring a B-type natriuretic peptide(BNP) blood test measuring the BNP level. This hormone dilates veins and arteries while regulating salt and fluid balance in the body.
In heart failure, the heart produces more BNP, which can be detected through blood tests and helps in early diagnosis and treatment.
3- What is the leading cause of congestive heart failure?
Congestive heart failure can be caused by coronary artery disease(CAD); it restricts blood flow to the heart, resulting in weak heart functioning. High blood pressure forces the heart to work harder, leading to its failure. Other factors like diabetes, heart attack, and valve disease are also responsible for congestive heart failure.
4- What lifestyle changes can be made to treat heart failure?
Small changes in your daily routine can improve heart health and lower the risk of heart failure.
- Exercise daily
- Limit alcohol and caffeine
- Have a balanced diet
- Low sodium and fat
- Manage weight
- Manage stress
- Monitor blood pressure
- Follow a proper sleep routine
5 – What are the four stages of heart failure?
American College of Cardiology (ACC) and the American Heart Association(AHA) have classified heart failure into four categories:
Stage A – no symptoms, but there are chances due to high blood pressure, diabetes, or a family history of heart disease.
Stage B– specific changes in heart shape but no symptoms of heart failure.
Stage C: noticeable symptoms like fatigue, breath shortness, and swelling due to improper heart functioning.
Stage D: symptoms start affecting your daily life, and you may require advanced treatment.
6- How to know my heart failure is getting worse?
- Rapid weight gain
- Swelling in the abdomen and legs
- Shortness of breath
- Irregular heartbeat
- Fatigue and dizziness
If these symptoms worsen, you should seek medical help immediately.

